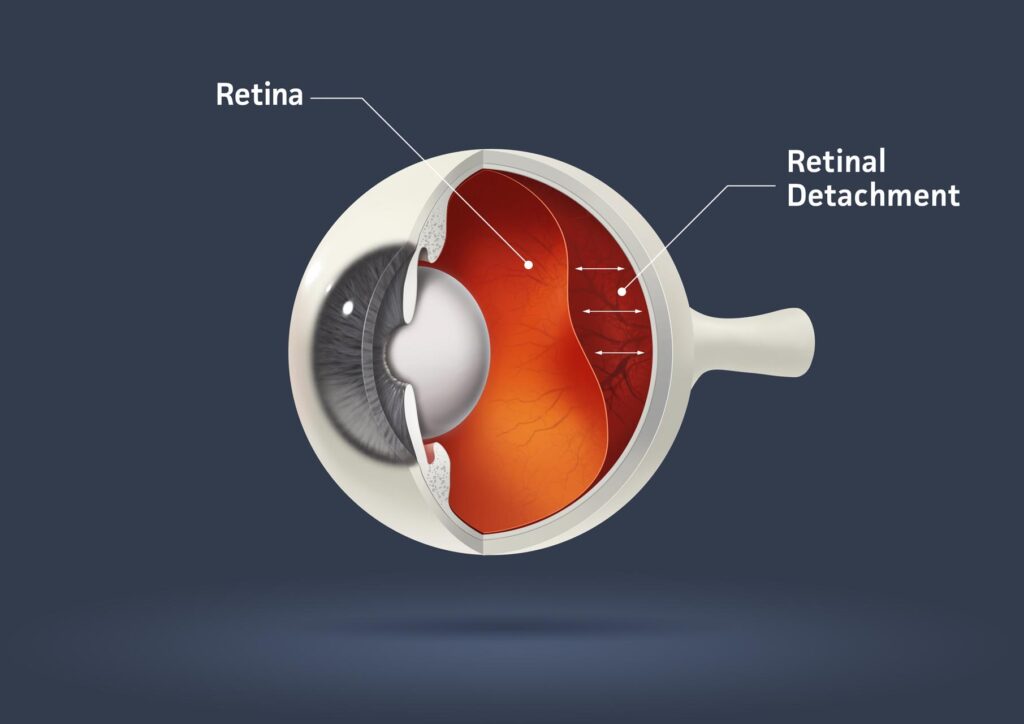
Retinal Detachment (Amotio)
What is the retina?
The retina is an essential part of the human eye. It is also called the inner skin of the eye and is the nerve tissue that is located on the inside of the wall of the eye. The light rays that enter the eye from the outside image are converted into electrical signals by light-sensitive receptors on the retina. Similar to a video chip in a camera. These electrical signals are then passed from the receptors to the brain. The brain then converts the signals into an image. Only an intact and correctly formed retina enables sharp vision.
What is a retinal detachment and what causes it?
When the retina detaches from the wall of the eye, it is called a retinal detachment. In most cases, the detachment of the retina from the wall of the eye is caused by a retinal tear. This can have the following cause: The so-called vitreous body, a transparent, gelatinous mass, is located in the rear chamber of the eye. When you are young, the vitreous completely fills the cavity, but it shrinks with age. It detaches itself from the back of the eye. In general, this shrinkage is not detrimental and is part of the normal aging process. However, it can happen that the vitreous body does not detach from the retina and then tears it with it as it shrinks. This then leads to a retinal tear. When such a tear occurs, vitreous humor leaks through the tear behind the retina. This lifts the retina off the wall of the eye. Retinal detachment generally lasts until complete detachment unless prevented by surgery. The retina that has detached no longer responds to light. Thus, a detached retina leads to blindness.
However, there are other causes that can lead to a tear or detachment of the retina. With normal aging, the retina can become thinner. The thinner retina can then tear spontaneously. Another reason may be near-sightedness (myopia). Myopic people have longer-than-normal eyes, making them more susceptible to retinal detachment. A mechanical impact, such as a blow to the eye, can also damage the vitreous humor and result in detachment of the retina. Certain eye surgeries can also cause retinal problems if the vitreous is jarred. Another reason for the detachment of the retina can be a tumour, an inflammation or even diabetes.
How do you spot a retinal detachment?
There are many patients between the ages of 40 and 70 who see threads, spider webs, mosquitoes, flies or other cloudiness in their eyes when there is a light background. This is best seen by looking into the calm water at a white wall. However, that’s no cause for concern. This phenomenon is due to the shrinking of the vitreous body and is completely normal. To the eye, these spots will not go away, but the brain will continue to block them out over time. However, if cataract surgery has been performed, these spots may reappear.
If you see flashes of lightning and stars in a certain area in one eye, this is a sign of a retinal tear. These flashes remain in the same place and do not travel. They are a reaction of the retina when the vitreous pulls too hard. If the tear is associated with bleeding in the eye, the eye will float like a flake of soot. However, there may be no symptoms after a retinal tear until detachment occurs. This becomes noticeable in the form of shadows in peripheral vision that become ever larger. The detaching retina no longer reacts to the light and thus the shadows increase.
Nowadays, ophthalmologists have numerous devices that make it possible to diagnose retinal diseases. The retina can then be examined in a variety of ways, allowing the specialist to choose the type and means of treatment to be performed.
What treatment options are there?
The success of the treatment depends on the initial degree of damage. Retinal tears and detachments can be resolved if treated early.
Treatment of retinal tears
Treating retinal tears is easier than fixing detachments. To treat cracks, the damaged area is closed with the help of a laser. This prevents the crack from expanding. The treatment is painless, no incisions are made. The laser is aimed at the area around the crack and coagulation creates a scar that closes the crack.
Another method, which is used less and less nowadays, is an operative method with a cold probe (cryoprobe). This procedure is performed under sterile conditions with local anesthesia in an operating room.
Treatment of retinal detachments
Surgery is required for retinal detachment. A distinction is made between external intervention and intervention in the eye.
With the external intervention, the first step is to remove the vitreous that has penetrated between the retina and the back wall of the eye. The back of the eye is pressed against the detached retina with a silicone band that is fixed around the eye. Then, using a laser or a cryoprobe, the area is coagulated to attach the retina.
Vitrectomy is surgery on the inside of the retina. This procedure is used when the retina has completely detached from the back of the eye. The vitreous is removed by severing it with a needle-like probe and then suctioning it out. In order to push the retina back into the correct position and if possible reattach it, gas, air or (rarely) silicone oil is injected. Then the retina thus attached is attached with a laser.
The key to restoring vision is whether the macula is detached or attached. The macula is the area of the retina with the highest density of photoreceptor cells.
The following factors significantly influence the success of the operation:
How much time elapsed between detachment and reattachment and where the damage occurred and the extent of the damage. After all, 40% of patients regain good vision after the retina is reattached. Otherwise at least a further degradation of the eyesight is prevented.
Follow-up treatment after the operation
It can take up to 6 months to fully recover, but only ointments or drops need to be applied. In a few cases, a second operation is necessary. If the refractive power of the eye changes as a result of the procedure, this can be compensated for with corrective lenses.