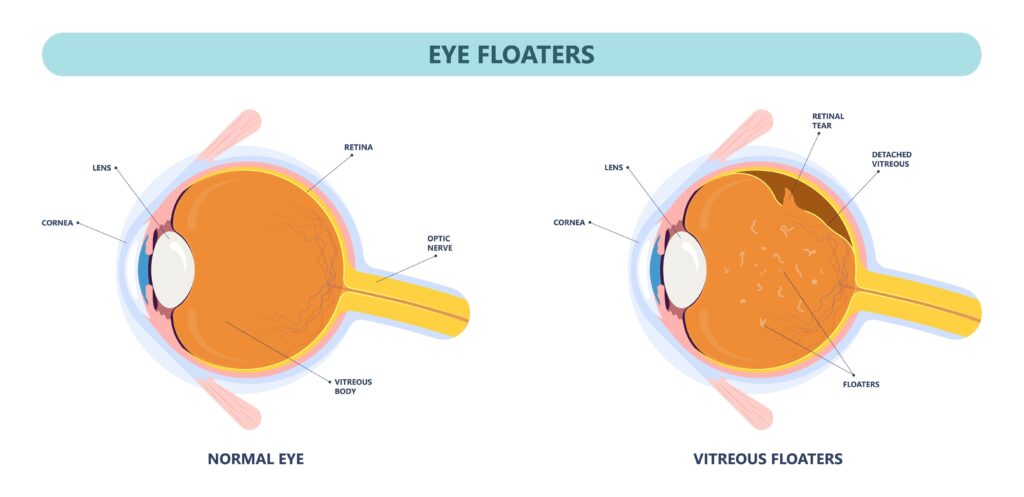
Vitreous body detachment
What is a vitreous detachment?
The vitreous body, a gelatinous substance in the eye, has the important task of filling the posterior chamber of the eye and supporting eye mobility. However, over the course of life, the water-storing power of the vitreous body can decrease, causing it to lose size and detach from the retina. This process is called posterior vitreous detachment and can be accelerated by injury or aging.
Mechanical irritation of the retina can occur during this detachment, which in the worst case can lead to detachment of the retina. This is mostly unproblematic. Part of the vitreous body is firmly attached to the retina. The vitreous body will also detach from the retina at these attachment points. This can take several days or even weeks. During normal eye movements, the vitreous body – flung back and forth like a deflated balloon – can pull on the retina. As a result, the retina is mechanically irritated, or even a hole is torn in the retina. In the worst case, this can lead to a detachment of the retina. The vitreous detachment is therefore nothing pathological, but a completely normal aging process. Most people are affected by it in old age. However, vitreous detachment can also occur earlier in life, e.g. B. with higher myopia, after an injury or bruise of the eye or after a cataract operation.
Causes, frequency, symptoms:
The retina, the most sensitive tissue in the eye, transmits light stimuli to the brain. However, there may also be perceptions of flashes of light or “seeing asterisks” caused by mechanical irritation of the eye without an actual light stimulus being present. This can be a sign of mechanical irritation of the retina. A ruptured blood vessel in the eye can cause vitreous hemorrhage, which is sometimes felt as “clouds” or “clouds.” In more severe cases, retinal detachment may occur, accompanied by a shadow in vision.
It’s important to see an eye doctor right away if you suddenly experience symptoms such as moving opacities, flashes of light, “ash rain,” or shadows in the peripheral vision, as this may indicate a retinal disorder, such as retinal detachment. In order to diagnose vitreous detachment, a thorough examination of the vitreous body and the retina is carried out with the slit lamp microscope and the ophthalmoscope with the pupil dilated by medication. It is important to note that dilation of the pupils can affect your ability to drive, so you should not drive yourself to the exam.
How is vitreous detachment treated?
In many cases, a posterior vitreous detachment cannot be treated. However, if a retinal tear develops, argon laser coagulation can be performed to close the tear. However, some cases may require more major surgery, such as suturing or even a vitrectomy, in which the vitreous is removed and the eye is filled with air, gas, electrolyte solution, or oil.
In order to detect a retinal detachment early, you should visit an ophthalmologist regularly. Between exams, one can do a self-test by closing the unaffected eye, looking at an object, and observing the fingers on the outstretched arms in the visual field without moving the eyes. The test should be repeated with both eyes to ensure that the fields of vision are comparable.